By Christopher Monckton of Brenchley
This column does not constitute medical advice. Check with your doctor. Many nostrums are being recommended, with varying justification, to reduce the harm from the Chinese virus. Some, like hydroxychloroquine, have side-effects and should only be taken if prescribed; others, like remdesivir, work (if at all) only during the early stages of disease; others, like the BCG virus against TB, have not yet been subjected to clinical trials.
However, early studies showed an interesting result, which the Marxstream media lazily attributed to capitalism’s imagined failures: the darker your skin, the more your risk from the infection. In Britain, all of the first ten doctors to die from Covid-19 were dark-skinned.
The pandemic has struck most severely above 35°N (editorial in Aliment. Pharm. Therap., and Marik et al. 2020), just as flu tends to end as summer comes. When the skin is exposed to the sun, the body makes Vitamin D3 more efficiently than through diet: salmon, tuna, mackerel, milk, some cereals, mushrooms and eggs all contain Vitamin D.
Vitamin D, used by the body to absorb calcium and grow bones, increases the production of antiviral proteins and decreases cytokines, the immune molecules known to cause a storm of dangerous inflammation, particularly in Chinese-virus patients. A shortage is linked to rickets, cancers, heart disease and weight gain. It is efficacious against many diseases:
Vitamin D deficiency is common not only in dark-skinned people, whose pigment blocks sunlight, but also in obese people, where the vitamin gets sequestered in fat cells; in those with Type 2 diabetes, where Vitamin D improves sensitivity to insulin; in the elderly, who avoid the sun and eat less; city dwellers, who see less of the sun; and men, who have lower Vitamin D levels than women in the winter. All of these groups are more likely to suffer severely if infected with the Chinese virus.
A recent study in Manchester found that average levels of vitamin D were 30% higher in summer than in winter and three times as high at all times in white people as in South Asians, who had less than a quarter of the 25 nanograms per milliliter that is regarded as sufficient.
Vitamin D3, in the form of gel tablets, is inexpensive and available without prescription, There are very few side-effects. A daily dose of 1000-4000 international units (25-100 micrograms) will maintain a sufficient Vitamin D level in most patients. The lower dosage is suitable for whites; darker-skinned people may need higher doses.
As already reported in this series, deficiency of Vitamin D3 is a long-proven risk factor for respiratory infections. The Chinese virus chiefly attacks the lungs. As Martineau et al. (BMJ 2017) showed in a meta-analysis of clinical trials involving more than 10,500 patients, rectifying Vitamin D3 deficiency reduces the risk of respiratory infection by 70%.
Recently, several commenters, notably William Astley and my good friend Dr Pat Frank, have provided additional evidence touching upon the efficacy of Vitamin D3 in keeping the pandemic at bay. Here is a summary.
Vitamin D supplementation could possibly improve clinical outcomes of patients infected with COVID-19, a preprint by Dr Mark Alipio of Davao Doctors’ College, Philippines (https://ssrn.com/abstract=3571484), reports retrospectively on 212 Chinese-virus cases. The Vitamin D level was found to be lowest in critical cases and highest in mild cases. Most of those infected had Vitamin D deficiency.
For each standard-deviation increase in serum 25-hydroxy-Vitamin D, the risk of a severe outcome was reduced eightfold, and the risk of a critical outcome was reduced 20-fold.
My noble friend Lord Ridley, reporting this result in The Times a couple of days ago, wrote: “Of 49 patients with mild symptoms … only two had low levels of vitamin D; of 104 patients with critical or severe symptoms, only four did not have low levels of vitamin D.”
Several doctors wrote to the BMJ last week drawing attention to Dr Alipio’s results: “Vitamin D biology is a mature well-researched field, dating back 100 years. Doses, and risks, within clinical parameters, are established and well quantified. Governmental intake guidance exists. Vitamin D deficiency is a medically accepted condition, requiring treatment.” In Britain, one in five are deficient in Vitamin D, which is why Public Health England recommends that everyone should take supplementation during the lockdown.
Evidence that Vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths (Grant et al., Nutrients, April 2, 2020) found that “through several mechanisms, vitamin D can reduce risk of infections. Those mechanisms include inducing cathelicidins and defensins that can lower viral replication rates and reducing concentrations of pro-inflammatory cytokines that produce the inflammation that injures the lining of the lungs, leading to pneumonia, as well as increasing concentrations of anti-inflammatory cytokines.”
The paper provided some interesting evidence that Vitamin D reduces Chinese-virus risk: “The outbreak occurred in winter, a time when 25-hydroxyvitamin D concentrations are lowest; the number of cases in the Southern Hemisphere near the end of summer are low; that vitamin D deficiency has been found to contribute to acute respiratory distress syndrome; and that case-fatality rates increase with age and with chronic disease comorbidity, both of which are associated with lower 25(OH)D concentration.”
Interestingly, the paper recommends much higher dosages than usual: “To reduce the risk of infection, it is recommended that people at risk of influenza and/or COVID-19 consider taking 10,000 international units per day of vitamin D3 for a few weeks to rapidly raise 25(OH)D concentrations, followed by 5000 international units per day.”
The paper also recommends doubling what had been regarded as the minimum threshold concentration of Vitamin D in the blood: “… raise 25(OH)D concentrations above 40-60 nanograms per millilitre (100-150 nanomoles per liter). For treatment of people who become infected with COVID-19, higher vitamin D3 doses might be useful.”
Patterns of COVID-19 Mortality and Vitamin D: An Indonesian Study (Rahasurun et al., April 26, 2020: https://ssrn.com/abstract=3585561) looked at 780 patients. “… the majority of the death cases were male and older and had pre-existing conditions and below-normal Vitamin D serum levels … with increasing odds of death. When controlling for age, sex, and comorbidity, Vitamin D status is strongly associated with COVID-19 mortality outcome …”
Vitamin D insufficiency is prevalent in severe COVID-19 (Lau et al., doi: https://doi.org/10.1101/2020.04.24.20075838) found that 11 of 13 intensive-care patients were deficient in Vitamin D, compared with only 4 of 7 not requiring intensive care. All Chinese-virus patients under 75 had Vitamin D deficiency.
Prevalence and correlates of Vitamin D deficiency in U.S. adults (Forrest & Stuhldreher, Nutr. Res., January 2011) studied almost 5000 patients and found that 42% were deficient in Vitamin D, but that 69% of Hispanics and 82% of black patients were deficient. “Vitamin D deficiency was significantly more common among those who had no college education, were obese, with a poor health status, hypertension, low high-density lipoprotein cholesterol level, or not consuming milk daily.”
Order now while stocks last. Some weeks ago, my lovely wife ordered a year’s supply from the United States, which never came. She ordered it from the UK instead and, at a small cost, now has enough to see her through until this time next year. I have been taking a 1000 IU (25 microgram) Vitamin D supplement every day for some years, and have had not so much as a sniffle in all that time.
Today’s charts show Sweden’s case-growth rate at zero for the first time, in line with the mean growth rate for the world excluding China and occupied Tibet. Aside from Canada, estimated active cases are declining in all the countries we are following.
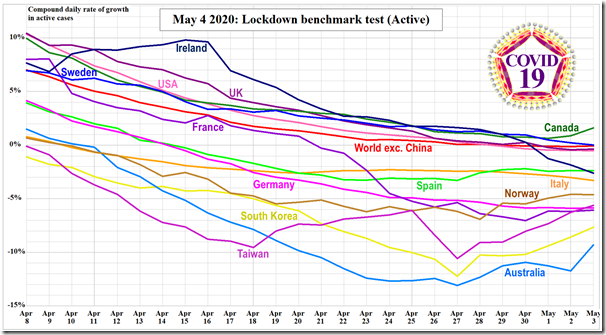
Fig. 1. Mean compound daily growth rates in estimated active cases of COVID-19 for the world excluding China (red) and for several individual nations averaged over the successive seven-day periods ending on all dates from April 8 to May 3, 2020.

Fig. 2. Mean compound daily growth rates in cumulative COVID-19 deaths for the world excluding China (red) and for several individual nations averaged over the successive seven-day periods ending on all dates from April 15 to May 3, 2020.
Ø High-definition Figures 1 and 2 are here.
Dr John Campbell has been harping endlessly about Vitamin D in his videos. I happen to think he’s right.
Either way, it’s not going to do you any harm to take it as a supplement. And it is not expensive.
Almost impossible to get now online in the UK. Just over a week ago I managed to get a year supply of D3 @ur momisugly 3k IU for myself and the wife, for the three younger members of family six months @ur momisugly 2k IU. If any of us gets even mildest symptoms all of us will up the dosage to 6k IU/day
https://www.amazon.co.uk/s?k=vitamin+d3&ref=nb_sb_noss_2
There are all sorts of people selling stuff on Amazon and Ebay, ok for shirts or books, not sure about medicines. I’m talking of the legitimate high street chemists e.g. Boots, Lloyds ph. etc.
I you want it, you get it, I got it this way within 3 days.
Cod liver you get there too.
I recognize several of the brands – Rite-Flex was the first one in the non-advertisement selections. (I take their chondroitin supplement, which I had checked out. Probably their D3 is also legitimate.)
In France smoked cod-liver is available in small tins like sardine tins. Great on toast or crackers. Tin contains the oil produced in cooking: which is a fair bit of the contents.
Don’t touch farmed salmon : it’s toxic ! Look it up if you are not aware.
This is a useful article on D3, largely posted here in comments recently but sadly CofB then goes back to more spurious misreading of his own graphs. Why he is not capable of reading what is in front of remains a mystery.
Firstly thanks for finally getting Sweden right, yesterday he was claiming Sweden was showing “no decline” despite dropping 8% to near zero.
But now we read “all countries” plotted are declining when in truth three are showing marked and sustaining increases in the last two or three weeks. Australia, Taiwan and S. Korea.
The two asian countries are exactly the ones which he has been applauding for their authoritarian lockdowns being a great success. Australia has also imposed strict quarantine on incoming travellers and thus avoided large scale infection.
What his graph actually shows is that this strategy has a downside: you have not beaten the virus, you can run but you can’t hide. They are forever at risk of a flare up in their still largely naive populations.
Once again, CofB sees what he wants to see and changes the facts to fit his preconceived ideas.
Yes, I’ll stop “whining” when you stop BS-ing everyone.
The two asian countries are exactly the ones which he has been applauding for their authoritarian lockdowns being a great success.
Be fair. Monckton of Brenchley has been applauding them for their authoritarian track-trace-isolate policies that avoided authoritarian lockdowns.
Whether they can maintain that level of invasive monitoring and intervention to an effective degree remains to be seen.
PJF, I see the point you are trying to make but they have been using authoritarian control AND lockdowns, just in a more selective manner so as not to shut down the entire economy.
The aim of not writing off your own economy is great but a strategy heavily suppressing infection, while attractive at the hospital gate, is not long term viable. A society cannot live in perpetual fear of an epidemic hanging over their heads, day after day.
It is not clear from the CofB “active” graph what the up tick in S.K. , Taiwan and Aus means. Is it good news : so few cases that firm reductions are fading back towards zero, or is it bad: a pick up in infections. If your metric does not tell you whether changes are good or bad, what use is it?
Better just look at daily new cases:
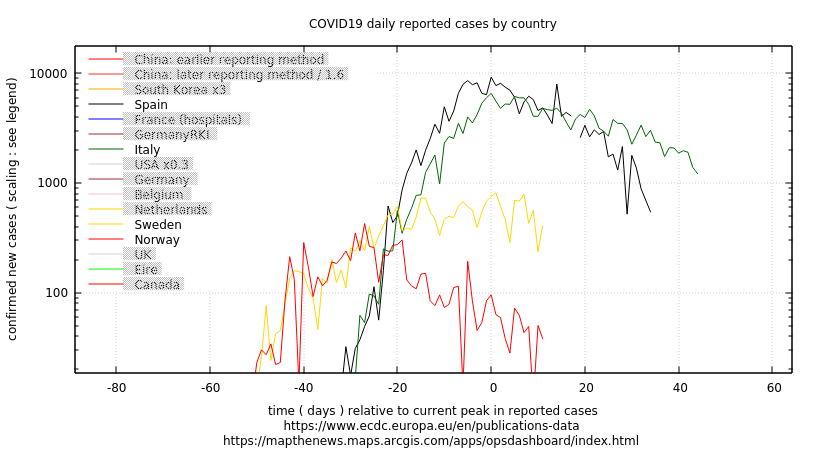
We can see that nothing bad has happened in Spain or Italy since they started relaxing confinement. That should be being closely watched by UK and USA as they struggle to work out which foot to put forward. Look at western countries which have been through it and played the crash test dummy , instead of yet more non validated models with speculative parameter tweaking.
My weekly averaging of rate of change of daily cases makes the Italian experience even clearer.

My cardiologist says that more than 4,000 IU/day could damage liver. He recommended 4k, I am taking 3k.
George
I take 1000IU D3 with every meal due to little exposure to sun. For many years. My “pill” is a tasty gummy with 2.5 grams of fiber, and 500IU D3 — two with every meal. I paid for the fiber and the D3 was a surprise bonus.
I ordered 500IU D3 pills for the wife a month ago but more expensive 5,000IU pills showed up. She decided to take three 5000IU pills a week.
My reading suggests more D3
than we take could be too much.
My cardiologist approves my taking calcium citrate with D3. I take 1000mg of each a day. I have been doing this for several years. I buy mine at Walmart, with prices of about $4 to maybe $8, depending on the size of bottle. I feel that at my age, 81, I probably need the extra calcium and the D3 makes it available for my body. I also take a multivitamin, again available at Walmart. They are all available at their internet sit.
That’s almost certainly utter nonsense. If you are mostly naked for two or three hours in the summer even at the sort of sunshine levels you get in the UK your body will generate 10 to 20,000 IU
RDA for supplements is set at the barest minimum to prevent death in most cases.
my rheumatology professor supplie me with a dry powder form of Vit D that was 20,000iu once a week
sure helped the aches and improved the mood.
another couple of things a hell of a lot of people are low in is Iodine(people dont remember the old goitres) and dont know to buy IODISED salt
the thyroid and related systems will uptake the fluorines if iodines not found, not a good outcome
magnesium is like VitD entire body needs for many processes,
and selenium
2 to 4 brazil nuts a day is plenty to sort that out
I dont know anyone who eats enough “proper food” a day to ensure adequate vitamin or mineral intake, no one has the time -OR money to afford it either
I’ve been taking 10000 IU D3 for a couple of years — my last blood test in Ireland showed >100 (not sure of the units; I think that they’d like to see at least 40, and past 100 they don’t quantify it) and my liver and renal function was great. Sadly I’ve got Splenic Marginal Zone Lymphoma — totally indolent at this stage, would never have known except for the blood tests — and my IgM antibody level is 0. I’m sure hoping the D level helps!
You may try https://www.docmorris.de/produkte/vitamine-mineralstoffe/vitamine/vitamin-d
it’s a online pharmacy
You can get over 15,000 IUs of D3 equivalent free by spending 10 minutes or so out in the sun without sunsreens/blockers/etc. (it’s a body process involving skin, liver and kidneys). All it needs is cholesterol and sunlight. If you’re on statins, it will still work. The only caution is to be sure not to sunburn since that’s cancer causing over time. After all, humans evolved walking around naked under the Sun.
If you need to, put on the sun blockers and screens AFTER you’ve got your dose of D.
Or go to a tanning booth. The full naked body only needs about 5 to 7 minutes.
Increasing Vit D3 via oral supplements takes weeks. Sunlight is quicker, the D3 produced is already “absorbed”.
Oh, and remember, word is that no healthy person, ever, ever died of an overdose of any vitamin.
Lots of studies on line since you should confirm anything diet/medical/etc., to your satisfaction including the pathways, the bio-med, etc.
And on those in CA, looks like your Governor may have stock in the vitamin industry by not recommending using the beach.
Good answer, with the exception of the bit about sunblockers. I don’t know about the US, but the majority tested in Europe actually contain carcinogens. If you’re going to use some blockers search out the ones which don’t of course.
Sun bathing is risky if you spend 6h per day stretched out a beach towel for 14 days on your previously unexposed skin.
No one is going to get skin cancer from 10min per day needed for vitamin D production.
“Oh, and remember, word is that no healthy person, ever, ever died of an overdose of any vitamin.”
That statement is wrong. There are cases. You have to be careful with lipophilic vitamins cause those can accumulate and the body doesn’t remove them fast enough when overdosed.
Vitamin D is a lipophilic one.
IIRC early Arctic explorers were poisoned by the very high levels of Vitamin A in polar bear, seal and walrus liver. A pound of polar bear liver can contain 9 million I.U.s of Vitamin A which is about 30 times a lethal dose.
“Oh, and remember, word is that no healthy person, ever, ever died of an overdose of any vitamin.”
Word is, eh?
That is how all the very best medical and nutritional advice is obtained, no doubt.
*rolls the eyes*
It sure would be dumb to think that if something is good, as much as possible must be better.
Get the right amount.
And make sure you get all the nutrients you need.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5986531/
Oh and that link was to only one of many studies pointing out what having too much vitamin D and calcium might do.
“Vitamin D in Vascular Calcification: A Double-Edged Sword?
No one has ever demonstrated that taking a vitamin d pill is as good as getting it from the Sun.
It is better than not getting any, is all one can say.
Vuk:
If you have a Wilko store near you pop in there (after waiting in line of course). I picked up a tube of VitD + calcium just yesterday. Seemed to have no shortage of all the usual vitamin tablets and cod liver oil capsules. The store staff at the door , checking people in one at a time , were also busy wiping down all the baskets with sanitizer.
I got mine from Tesco
Need to take drops under the tongue…
…I agree
I have stated this elsewhere, but it bears repeating: zinc is one of the other vital components to fight this virus. And there is no greater source of zinc than oysters. Three ounces contain 7 times the minimum daily requirement. And they’re sooooo delicious!
In addition to taking zinc one should also be sure to get zinc ionophores, or nutrients that move xinc from the bloodstream into the cells where it can work. Epigallocatechin-gallate (ECGC, abundant in green tea) and quercetin (abundant in onions and other some vegetables) are two you can get from a normal diet. Quinine is another, but there is not much quinine in commercial “tonic” and chloroquine &/or hydroxychloroquine require a prescription (besides having risks).
It seems to be pretty easy to take too much zinc (it has a months long half-life and can accumulate in the body) so one should be careful with it. Those like me who take eye vitamins should read the label, you are probably already taking some zinc.
Milk — It does a body good. I drink a gallon or more a day. Always have and always will. But it don’t mix well with beer!
I’ll up the intake when the tomatos start coming in. A couple of tomato sandwiches and a BIG mug of milk is heaven!
So wish I could like I use to, but I’m severely allergic to dairy. Live in a northern climate and have darker skin tone that can go very dark with sun in summers.
Which in the last few decades I’ve avoided to the max, think now I’ll start going into the sun directly without so much fear or sunscreen.
I was told to take calcium – so I have for most of my adult life; but I got osteoporosis anyway.
No one explained that I needed Vit D to absorb the calcium – now taking both in the last couple of years, but I will now increase my Vit D IU per day to 4000 up from 2000 recommended on the bottle.
In addition to your calcium supplement you need to do load bearing exercises…some weights perhaps,
Without load bones wste away
Dr Roger Seheult also promotes vitamin D in his Medcram videos.
Actually, the only medical professional who I haven’t heard mentioning vitamin D is the UK CMO.
Preliminary data ….. showing severity by vitamin D and vitamin D deficiency by race. If I new how to make them pictures I would, but they are PDF … help section says has to be jpeg.
https://www.grassrootshealth.net/wp-content/uploads/2020/04/Vit-D-COVID-Severity-0421.pdf
https://www.grassrootshealth.net/wp-content/uploads/2020/04/NHANES-bar-graph-adults-by-race-2013-14.pdf
Indonesian study on this subject:
https://papers.ssrn.com/sol3/Delivery.cfm/SSRN_ID3585561_code4138052.pdf?abstractid=3585561&mirid=1&type=2
I am a believer. Daily doses of D3 for me.
they are all …all over the map with this
I don’t care what it is…there’s always someone saying the opposite
May 1, 2020
Vitamin D: A rapid review of the evidence for treatment or prevention in COVID-19
VERDICT
We found no clinical evidence on vitamin D in COVID-19. There was no evidence related to vitamin D deficiency predisposing to COVID-19, nor were there studies of supplementation for preventing or treating COVID-19.
https://www.cebm.net/covid-19/vitamin-d-a-rapid-review-of-the-evidence-for-treatment-or-prevention-in-covid-19/
I think I would ignore this web site. They said they looked at the medrxiv site. If they did they should have seen the study referred to in the post yesterday.
I think this a case where you need to look carefully as what they say and what those terms mean medically.
” There was no evidence ” and “nor were there studies of ” probably means there were no clinical, randomised , double-blind studies of COVID vs D3. That may be factually correct.
It’s bit like similar claims about HCQ. They have studiously avoided doing any tests which fulfill these criteria, so they can still claim there is “no evidence” it works, despite widespread use in Spain and Italy: two countries with the best proportion of recovered COVID-19 patients.
Don’t think you’re being paranoid because you think they’re out to get us. They are!
I did not say they were not seeking to mislead. I said you have to look carefully at what they are saying to interpret what it means. Most people will not look closely and will be mislead. They can always claim to have made technically factual statements.
They recommended vitamin D supplementation in any case, but absence of evidence is not evidence of absence, as we all know.
This is of course anecdotal but here goes. For 3 consecutive winters beginning with Dec. 2016 through December 2018, by late January early February I developed a form of bronchial infection that seemed to hang on for weeks and had to take a 10 day course of antibiotic. Somewhere I read that Vitamin D helped support the immune system and began to supplement with D3. I am 77 and now understand that my skin is less likely to produce as much of the vitamin and because of squamus cell skin cancers and pre-cancerous spots I avoid sunshine in summer wearing sunscreen and sun sleeves when golfing. I took a 5000 IU capsule once a day until October 2019, when I doubled that, taking one in the morning and one in the evening. I still do and my research indicates this dosage is tolerated in healthy individuals. I have maintained high aerobic fitness for over fifty years adding resistance exercises for the last 35. When Covid-19 seriously came to light in late February this year it dawned on me that for the first time in 4 years I had no bronchial issues and only one brief cold since the last occurrence in 2019. With all the talk about anti-bodies I wondered if my bouts with bronchitis had given me protection. Not so. Based on the information here and a previous post on WUWT, I believe that vitamin D3 does support the immune system. Additional D3 was the only significant change in my diet, supplementary or lifestyle practices in the last year. Not taking any chances though. I wear the mask and maintain physical distance, going out only when necessary.
Also, potassium deficiency might be a factor, according to this piece:
https://www.medrxiv.org/content/10.1101/2020.02.27.20028530v1
My dermatologist, when I asked him 15 years ago for any nutritional recommendation, without hesitation said “Vitamin D”. It was years later when D appeared on my yearly blood panel, and my personal physician ordered 4000 IU per day. Since then I have avoided recurring moderate depression, and stopped catching colds once or twice per year. Here in in Nevada, skin cancer is a plague, and direct sunlight on the skin to be avoided.
PS buy your Vitamin D from a reputable source. My doctor refers to ConsumerLab for testing of supplements, and recommends Costco or Trader Joe’s generally. I buy Kirkland (Costco) 600 count 2000 IU D3 gel caps.
Depends on your skin and family history. I get about an hour a day in the sun here in Henderson. No sunscreen. I started a couple of months ago when we had the first spell of warm weather, at 10 minutes per angle. Now I’m up to at least 30 minutes front and 30 minutes back. Feels good.
“No Salt” salt substitute is an easy way to get potassium.
Reading your article about hypokalemia, it seems that they are citing low potassium as a biomarker. Perhaps the low potassium is an effect of kidney function, not a direct cause of the severity of infection. It does say that, hypokalemia being identified, supplementation is effective.
Either way, it’s not going to do you any harm to take it as a supplement. And it is not expensive.
It may do you some harm if you believe it will save you, and you fail to do the things that will actually save you.
Vitamin D level is probably a very good indicator of cardio-vascular fitness, which is generally obtained only by exercising outdoors in daylight, so maybe the advice should be to get fitter, rather than to pop another pill.
Dear Lord Monckton, please write about Corona and smoking. Smoker were 5% (between 3 and 11%) of Corona-hospitalized in France and China. Non-smokers around 95% of infected. There seems to be a low cost prophylaxis is leaving the house with 1 cigaret smoked. The smoker record should be available from patients hospital admission records.
Maybe even marihuana smoking may be beneficial in lung protection – this would be a surprise.
Lots to check out.
Heavy smoking residues apparently stop the CV virus penetrating the lungs’ cells.
In that respect there’s been no comment about vaping nicotine along with vegetable glycerine and propylene glycol in the e-juice where nicotine is the common element. It would be ironic if it’s the smoke from burnt vegetable matter that offers some added protection.
Smoking likely causes involuntary social distancing and masks some symptoms, cough, loss of smell and taste. (I am a smoker)
Honesty is the best policy. Of course insanity is a better defense.
🙂
A diet rich in beans would accomplish the same thing, and most likely be healthier…
Smoker here, too, although oddly enough it doesn’t particularly affect my sense of smell or taste very much, if at all.
Except at the onset of allergy season, when it is other things. The entire family has the full set of symptoms for CoViD-19 – except fever. Sigh…
“A diet rich in beans would accomplish the same thing, and most likely be healthier…”
… and also helps with social distancing.
Or maybe smoking is a proxy for being outside in the sun (ergo Vitamin D again)?
Is there an inverse correlation between smoking and obesity? Isn’t weight gain common when someone stops smoking? Smokers may also spend more time outside in the sun.
Our German virologist Drosten can’t and will not explain these smoker data, there must be a mistake.
😀
From what I remember, possibly wrong, 25 nanograms per milliliter is a bare minimum for sufficiency, and 40-80 is preferred. I take 4000 IU daily and can barely keep my annual test results above 40.
I take 4000 IU daily, and my NG / ML is 43.0. I’m 65 years old, not obese, live in sunny NV but avoid direct sunlight as much as is practical.
5 – 15 minutes, 2 – 3 times a week, hands, arms, and face. (No sunscreen, though.) Although I presume more for darker people.
There is a distinction between Vitamin D supplements and Vitamin D3 supplements. D3 is safer in large doses.
As an aside, Sarasota County opened the beaches last week and the adjacent parking lots today.
I spent a couple of hours there this afternoon, sunny and warm with a steady breeze coming in off the 80F turquoise blue Gulf waters.
Not a bad way to get your Vitamin D.
Not a bad way to get your Vitamin D
The best one 😀
What about Russia? Are they not suffering from vitamin D deficiency?
In Putin’s Russia, Vitamin D gets you!!
sorry- couldn’t resist.
The bigger question: do we trust anything coming out of China or Russia?
What about Finland?
They are alive!
I know, staying here with my wife.
But for the moment longing to our Island ( in the sun?) in Sweden.
Vladimir Putin’s popularity slumps as coronavirus ravages Russia and country sees more than 10,000 new infections for second day in a row
Don’t worry, the FSB will whip it up again.
Putin has finally run into an opponent that an assignation squad can’t take care of.
My wife is in Russia at the moment caring for her mother. She is in Tula (approx 500K people). I think that Putin’s popularity slump is also caused by increasing costs of many items particularly food. I have asked her how many cases of Covid19 have been seen in Tula. She says very few but doesn’t have more definitive numbers. Never the less there is social distancing and masks by govt decree.
I have asked her in the past what people think about Putin meddling in the middle east, Iran etc when there are huge problems in Russia. She wont comment perhaps from fear of being overheard. When I have been in Russia people will complain about Putin and the govt in private if they trust you.
Russia has exposed people to UV light for years, especially in Siberia. I remember a NatGeo article 30 years ago showing them zapping young kids in a remote Siberian town in the middle of winter.
That’s not to say everyone partakes there now with light, especially with pills as options, but they were addressing the issue.
Yes, it’s leading cause of collusion.
I can remember being force-fed cod liver oil in winter back in the 1940s and children in UK, US etc. were exposed to therapeutic artificial UV well before that:
https://mashable.com/2015/08/07/sun-therapy-children/
And malt extract fortified with Cod Liver Oil. I still take Cpod liver Oil in capsule form.
Thanks, my vitamin d was low last time I had blood work. Dr recommended vitamin d supplement. I started then stopped. I think I will start again.
4000 IU D3 per day, can’t go wrong. Do your homework for quality product.
I do 5000/day.
The Dr. tested me at 71mg/dl. About 45degrees Northern hemisphere.
Cod liver is a very good source for vitamine D, I got it regulary as child in winter to prevent rachitis. If one like it…..
It is good to have this discussion about vitimine D, but it in a way is old news.
Below is what my Dr. read to me back in March.
•Vitamin C 500 mg BID and Quercetin 250-500 mg BID
•Zinc 75-100 mg/day (acetate, gluconate or picolinate). Zinc lozenges are preferred. After 1 month, reduce the dose to 30-50 mg/day.
•Melatonin (slow release): Begin with 0.3mg and increase as tolerated to 2 mg at night
•Vitamin D3 1000-4000 u/day
The real story is how the WHO/CDC et all fostered an incorrect treatment on the world that killed a lot of people. From evms…
Our long-standing and more recent experiences show consistently successful treatment if traditional therapeutic principles of early and aggressive intervention is achieved, before the onset of advanced organ failure. It is our collective opinion that the historically high levels of morbidity and mortality from COVID-19 is due to a single factor: the widespread and inappropriate reluctance amongst intensivists to employ anti-inflammatory and anticoagulant treatments, including corticosteroid therapy early in the course of a patient’s hospitalization. It is essential to recognize that it is not the virus that is killing the patient, rather it is the patient’s overactive immune system. The flames of the “cytokine fire” are out of control and need to be extinguished. Providing supportive care (with ventilators that themselves stoke the fire) and waiting for the cytokine fire to burn itself out simply does not work… this approach has FAILED and has led to the death of tens of thousands of patients.
The systematic failure of critical care systems to adopt corticosteroid therapy resulted from the published recommendations against corticosteroids use by the World Health Organization (WHO), the Centers for Disease Control and Prevention (CDC), and the American Thoracic Society (ATS) amongst others. A very recent publication by the Society of Critical Care Medicine and authored one of the members of the Front Line COVID-19 Critical Care (FLCCC) group (UM), identified the errors made by these organizations in their analyses of corticosteroid studies based on the findings of the SARS and H1N1 pandemics. Their erroneous recommendation to avoid corticosteroids in the treatment of COVID-19 has led to the development of myriad organ failures which have overwhelmed critical care systems across the world.
I have tracked down data to support all this and posted here before. This is the story that no one wants to cover. Down load from
evms.edu/covidcare
Above is from page 9/10
I just watched an hour long interview with Dr. Marik. I’d post it here, but the interviewer was too annoying. His protocol makes a lot of sense. If you have a good video post it. He’s apparently a very accomplished doctor in critical care with more published papers on the topic than anyone in the US.
Hey,
Where did you find video?
Came across a very disturbing report of a death where I want to move jackson wy, sounded like nyc
It was a video about Dr Marik’s treatment for sepsis. He mentioned that sepsis patients in ICU are not tested for serum vitamin C level, but those that have been had scurvy levels. The interviewer was ZdoggMD; highly annoying.
Sure wish some one would do full blown article on his protocol here.
I trust my Dr’s reference
It is very hard to get traction on it anywhere I have tried.
Just keep hammering away with facts. Look how long it took to get an article on vitamin D. It takes time to overcome conditioning and embrace a paradigm that includes epigenetics and iatrogenic disease.
I did find this.
https://youtu.be/sKExxcD26_I
Why the EVMS protocols must be considered
To the moderators on this site, what the hell does it take to get the fiasco in NYC and the solution as a top story on this site….
one reason for not using the cortisols was that they do lower the immune respone ie how they stop cytokine storms
they were worried they stop the immune response to fight the virus as well
fine line between whats going to kill you really
far of lawsuits is also a huge factor
follow the written protocols is what they do regardless of what they see, too often
like the massive hate against IV Vit C in spite of evidence it saved lifes for H1N1 patients
Just found a news article on protocol
https://spectator.org/a-report-from-the-front/
It was just updated. This dr developed HAT sepsis treatment
Chinese were using modified vs of HAT
Several years ago, the University of Toronto did a study of the Vitamin D levels in its students at the end of the winter.
Every single non-white student tested was significantly Vitamin D deficient. Every single one! (Many white students were deficient as well at this time of year.)
Please remember that vitamin D is NOT safe in overdose – it is the most effective rat poison on the market !
For more information on that, see
https://vitamindwiki.com/Name+a+rat+poison+crucial+to+health+and+safer+than+water
“Humans need about 4,000 units of vitamin D a day (from all sources). Ten times that amount, 40,000 units, is very safe in a single dose”
https://www.rootcausemedicalclinics.com/blog/is-your-vitamin-d3-supplement-toxic/
“The danger lies in the need to balance your vitamin K2 level with D3.”
https://www.drugs.com/answers/cholecalciferol-is-main-ingredient-in-rat-poison-336757.html
danger to cats and dogs too
“4,000,000 IUs (4 million IUs) given to a human. According to research, that amount could endanger your health, but not kill you.”
Years ago, my GP gave me a D3 presciption.. 7 weeks, 1 dose a week, 50,000 IU. It brought me up into the normal range.
Here in Texas, the Walgreens carries 5000 IU gelcaps, very inexpensive, and in moderate quantities. From that, possible to manage to any specific serum concentration desired.
This weekend, I cut bamboo on the property. No supplements required 🙂
Which is why people should take the precursor D3. Then the body will regulate the amount that is converted into Vitamin D.
Susan
There is nothing that is not poisonous if taken excessively. Fraternity pledges periodically die from drinking too much water. Pure oxygen can be dangerous; It will be fatal if one is using an oxygen re-breather and go too deep. Even breathing pure nitrogen will kill you; there has to be some oxygen along with it.
“The poison is in the dose.”
Paracelsus
That would suck, to die periodically. Ban Dihydrogen Monoxide now!
If done repetively, a learning experience.
You are assuming that a frat’ is capable learning. 🙂
Note that I was not talking about a particular frat’ pledge. I was using the generic, plural form. Either way, no great loss. 🙂
I have been and still do take between 8K IU and 10 thousand IU every day. For like the past seven plus years. ALSO , Please, vit K complex . High dose D 3 needs the K complex. I started at 37 and now is 80. Took over five years and testing. Actually to get to 80 I took more than 10k iu with k complex. Before my 80 level it was 67. Six months between test. I would guess , only 4iu would test less than 50 on the Hydro scale. I use to really suffer with cold, and flu. I still cycle cold bugs. Very mild. Five thousand with K complex is really the starting point. Testing important but do not fear taking too much. Dr Mercola and The Life Extension, are two good information sources . LifeExtension.com (can buy on Amazon) is the brand I trust. Been using LEF products over fifteen years. They test what they sell. Do not take D3 without the K complex.
You make an important point. D3 should be accompanied by K2 which apparently regulates calcium in the blood. I think it has to do with spurs and calcification of the arteries in old people of which I am one. (A comment here by an MD who knows what he’s doing would be good.)
quite a few cardiologists have warned about taking too much calcium leading to hear issues.
800mg a day MAX and 600 for women
if you do any weight bearing excersize then bones will draw in calcium and strengthen,
no excersise and lesser uptake of course.
women often get handed calcium for osteoporosis or pre osteop
excersize would be the better option
I found Dr Seheult’s routine video very useful : https://www.youtube.com/watch?v=NM2A2xNLWR4
Willaim Astley’s posts drew my attention to Vitamin D3. I looked into them, and they seemed credible.
In doing so, I checked the literature for correlation of Vitamin D3 and Covid-19. Several papers turned up connecting infection and death rates with low serum Vitamin D3, especially 25(OH)D, see here and here.
My thanks to Chris Monckton for putting it all together. His series of posts on the progress of the pandemic and inter-country comparisons are a tremendous service, and have been a lamp of rational sanity of a world driven half-mad by fear-mongering.
JOIN THE REVOLUTION!!!
This one, brilliant article will, on its own save many lives.
We must spread it far and wide, starting with family and friends. If enough people do this we will flatten all the curves. Then, the few people that catch the China Virus (CV) can be treated and the rest of us can get back to work, back to normal.
The effects of vitamin D on the renin-angiotensin system
“Angiotensin-converting enzyme 2 (ACE2) is an enzyme attached to the outer surface (cell membranes) of cells in the lungs, arteries, heart, kidney, and intestines. ACE2 lowers blood pressure by catalysing the hydrolysis of angiotensin II (a vasoconstrictor peptide) into angiotensin (1–7) (a vasodilator).”
“Angiotensin II leads to increased water and sodium reabsorption in the kidney and vasoconstriction. Mounting evidence indicates that vitamin D regulates the renin-angiotensin system. An inverse relationship between the blood pressure and serum 25(OH)D levels has been documented in a number of the epidemiological studies (4,5). In a cross-sectional study, Forman et al. explored the relation between 25(OH)D and the renin-angiotensin system in 184 individuals with normal blood pressure (6). Compared with vitamin D-sufficient individuals, those with vitamin D deficiency and insufficiency had greater plasma angiotensin II levels and a trend for higher plasma renin activity. In addition, the activity of the renin-angiotensin system in the kidney, as measured by the renal plasma flow in response to angiotensin II infusion, was greater in vitamin D-deficient than in vitamin D-sufficient individuals. These results suggested that decreased plasma 25(OH)D levels were associated with increased activity of the renin angiotensin system. Resnick et al. investigated the relation between the plasma renin activity and calcium-regulating hormones including calcitonin, 1,25(OH)2D3 and parathyroid hormone in 51 individuals with essential hypertension (7). An inverse relation of the serum 1,25(OH)2D3 level to the plasma renin activity (r= −0.65, P< 0.001) was observed. This study corroborated a link between calcium homeostasis, vitamin D metabolism and the renin-angiotensin system."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3999581/
Prophylactically, I recommend melatonin at a dose of 6 mg / day for people over 50 years of age. Melatonin as the peak hormone regulates the endocrine system and is an extremely powerful antioxidant.
Coronavirus deactivates the ACE2 enzyme in the lungs, which leads to narrowing of the blood vessels in the lungs and pneumonia.
Thanks, Christopher. I’m a D3 user myself, currently 3000 units. Your articles are always informative and a pleasure to read.
This is absolutely unbelievable. We have found the biggest scandal in scientific history.
So in three weeks, looking for a solution to the covid virus, we have found…
The ‘cure’ for Covid virus…
IS to correct our population’s deficiencies, using drug store available supplements .
In the US (and in almost all developed country) more than 40% of the population is Vitamin D deficient.
“Vitamin’ D is a proteohormone that turns genes on and off in 200 processes , in our body, which we are aware of now. 80% of our Vitamin D comes from sunlight. In Northern countries 6 months of the year it is not possible to make Vitamin D from sunlight.
https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3585561
Vitamin D status (OR=7.63; p<0.001). When compared to cases with normal Vitamin D status, death (William from the covid virus) was approximately 10.12 times more likely for Vitamin D deficient cases (OR=10.12; p60 ng/ml being most protective.
https://www.grassrootshealth.net/wp-content/uploads/2016/03/grh-lappe-cancer-journal.pone_.0152441.pdf
Other studies have found a similar reduction in risk for individual cancers [3–13]. Lowe et al. demonstrated in a hospital-based case control study that women with serum concentrations of >60 ng/ml had an 83% reduction in breast cancer risk compared to women with concentrations <20 ng/ml (P30 ng/ml compared to women with concentrations 29 ng/ml compared to women with concentrations <18 ng/ml (OR = 0.45, 95% CI: 0.250.81) [12].
This single graph, summarize this key issue.
https://www.grassrootshealth.net/wp-content/uploads/2017/05/disease-incidence-prev-chart-051317.pdf
Patterns of COVID-19 Mortality and Vitamin D: An Indonesian Study
https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3585561
Roughly ball park = 60% reduction in total country health care costs. (We need also to correct the population’s Zinc and Magnesium deficiency)
It appears that our cells, when we are at sufficient Vitamin D levels, use the Zinc to stop the covid virus from connecting to the ACE-2 connection in our cells. That stops replication.
Where deficient means the entire population, must take Vitamin D supplements of 4000 UI/day to reach the 40 ng/ml to 60 ng/ml level which has been shown along with calcium supplements to reduce the incidence of cancer by 70%.
82% of the Blacks in the US are Vitamin D deficient. That explains why more than twice as many Blacks in the US die of HIV and of Covid, than white people.
https://www.cdc.gov/hiv/group/racialethnic/africanamericans/index.html
HIV and African Americans
Blacks/African Americansa account for a higher proportion of new HIV diagnosesb and people with HIV, compared to other races/ethnicities. In 2018, blacks/African Americans accounted for 13% of the US populationc but 42% of the 37,832 new HIV diagnoses in the United States and dependent areas.d
If you want to see unbelievable.
Welcome to the Machine. Obviously a major factor in NYC’s high mortality. After watching this, will people still be able to think that all mortality associated with this virus is caused by the virus?
She mentions towards the end once instance where ventilator PEEP was dialed up to 25, which she said can blow out lung alveoli. Nutcracker lung
https://twitter.com/IvoMd/status/1255848198175961095
A survey of covid treaters shows low confidence in ventilators using ARDS protocol. They prefer high flow oxygen treatments, but many hospital administrators and doctors won’t allow such because they are more concerned about aerolsolization of virus than patients’ well-being.
Sermo Reports: 50% of Highly Experienced COVID Treaters Believe COVID-19 Is More of an “Oxygen Failure” Disease vs. a Respiratory Disease Leading to ARDS; 48% Believe Ventilators Used Too Rapidly
https://www.businesswire.com/news/home/20200504005250/en/Sermo-Reports-50-Highly-Experienced-COVID-Treaters#.XrCcH92Y0O8.twitter
Continuing on this thread,
Compare death rates (per 1M people):
NY: 1,376
CA: 68
https://nypost.com/2020/04/28/andrew-cuomo-refuses-to-face-facts-on-nursing-home-coronavirus-horrors/
Opinion
editorial
Andrew Cuomo refuses to face facts on nursing-home coronavirus horrors
By Post Editorial Board
April 28, 2020 | 7:37pm
Not content with refusing to admit his team has made a mistake in forcing nursing homes to take in patients infected with the deadly coronavirus, Gov. Andrew Cuomo has taken to answering questions on the subject with insults.
In the meantime 200000 old people and others with preconditions like cancer influenza ect, die EACH DAY and we have closed the whole world for a nothing burger virus my view anyway. This virus should have been left to do its thing!. By doing lockdowns yes many very old people with preconditions will die but by extending this many more will die for economic reasons estimated world unemployment now about 2,000,000,000 BILLIONS. Deaths from this will superpass the virus dramatically this has been the most ignorant stupid human response ever again Eistein was correct. Sweden seems to be doing OK with no lock down. I aint worried about Vitamin D live in Central South America years ago plenty of Sun heat and Vit D. I think Mockton would be correct about Black people living in countries with NO SUN such as Britain may suffer a severe deficiency and make them susceptible because they are in an environment not suitable for their physiology. People should not be living outside the subtropics a very basic premise thats why half the USA wants to live in Florida, Texas or Brazil! cheers my 2 cents worth
I have been saying all along that although I understand the desire to protect the healthcare systems from being overloaded, we are going to pay a heavy price for this somewhere down the line. There will be increases in mental disorders, (there have already been suicides here in the UK), depression, economic consequences, as well as the disgusting, communist style ‘informant’. I also wonder just how many of our freedoms will be held back? I’m not suggesting everywhere will suddenly become North Korea of course, but politicians do like power, and they do so hate giving it up…
“others, like the BCG virus against TB, have not yet been subjected to clinical trials.”
Good that you mention that. The BCG vaccine has been in use except in Italy, the US, and Canada. Some countries that did no longer do. There was a study which found that the difference in incidence and mortality of covid-19 was ten fold.
https://www.youtube.com/watch?v=LWsgbgz5euc&t=19m34s
https://www.urotoday.com/recent-abstracts/covid-19-and-genitourinary-cancers/120475-bcg-vaccination-policies-make-a-ten-times-difference-in-covid-19-incidence-mortality-new-study.html
I think you can think of voluntary vaccinations for medical staff with BCG to stimulate the immune system.
bcg was stopped for aussie kids in the 80s
nurses in highrisk areas etc still get it
presently a 4k nurses trial running in aus with the bcg bax
nothing on results etc yet
the vax has around a 20yr effective rating
I tailor my D3 capsule intake with annual climate change phenomena. At least in the annual global warming periods, I can save a couple of cents by taking less.
D3 is inexpensive-a cheap experiment, which reminds me, it is time to walk up to get some more after the rain that Tim Flannery said would never fall again ends later today.
Vitamin C is also a cheap experiment, but avoid the cheap unbuffered ones. Chewing too many with the direct ascorbic acid can erode the hell out of your teeth. Had such a case a number of years ago-atypical pattern of tooth erosion. The patient was mortified that so much damage was done in the quest to be more healthy.
james
The old homily, “Moderation in all things,” has much to recommend it.
… except in moderation itself.
Steven
I’ve wondered if moderation can be taken to an extreme.
Give the kids D3 and send them to school
Ask the pediatrician first, of course. I wonder why the kids are so resistant to COV-19. Is it because they’re not D3 deficient?
Well, you could require that all kids play outside in sunlight for couple days getting average of two hours of sunlight per day or if they not been outside, give them some D3 or have them drink some milk with d3 added, or eat eggs for breakfast.
Probably most kid are not deficient in D3, but don’t want there to be, say, 5 to 10% who might be- also fat kids could be more deficient than others. And probably don’t want to focus on just fat kids.
UV-B is required to convert cholesterol to Vitamin D in the skin. Since UV-B has a tough time getting to the surface of the Earth through the atmosphere and clouds, exposure with the Sun high in the sky and no clouds is the best time. The more skin you expose, the more Vitamin D is produced. One study showed in Oslo, Norway during June 30 minutes of exposure created from 10,000 to 20,000 IU’s. Since it is fat soluble, a few days a week is all you need in the high summer. After that, it takes longer until the Sun is so low you get no benefit. Living in the lower latitudes extends the time.
So take it all off and lay out when the opportunity presents. Just be a little careful with anything you don’t want to get overexposed, if you know what I mean.
Now I know why I feel so good when sailing in the sunshine at my favourite beaches in Thailand in January/February. It has to be all that Vitamin D!