By Chris Gillham
As one of the audit team for Jo Nova’s blog, I have been looking at the question of whether lockdowns work and their potential suppression of communicable diseases other than COVID-19.
Since the current pandemic only began killing people this year, there is no previous year with which it can be compared. However, lockdowns – to the extent that they work – will work not only against the current COVID-19 infection but also for other viral infections.
Take influenza as an example. The World Health Organization monitors positive and negative influenza notifications from laboratory tests in various countries (https://www.who.int/influenza/gisrs_laboratory/updates/summaryreport/en/), and this seems to be about the only up-to-date data on their website. So we can compare the flu test results in relevant post-lockdown weeks in 2020 with flu results in 2019 to see whether there is a marked difference.
Since the WHO publishes them, it might be assumed that these laboratory test results have some correlation with community influenza numbers in the different countries.
I have selected 17 countries based partly on their population size and prominence over the past few weeks in the COVID-19 crisis, and partly on whether or not they supplied sufficient weekly reports within the timeframe. My analysis starts in week 14 of 2019 and goes to week 18 of 2020, which was at the end of April. Their total influenza test positives can be presented graphically but are constrained by the most recent notifications, the US a laggard with its last notification in week 14 2020.
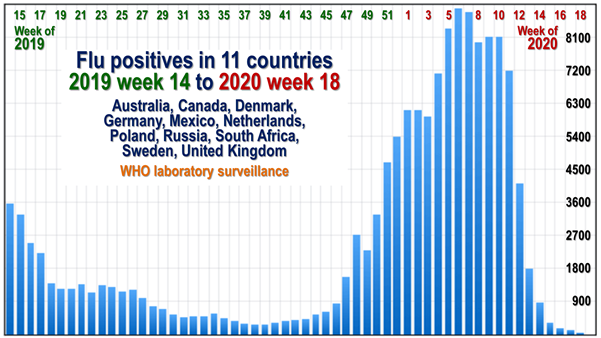
Fig. 1 shows flu positives in 11 countries with the most up-to-date data from week 14 of 2019 to week 18 of 2020. The significance of this graph is that normally the worst of the winter flu epidemic is over by week 14.
However, separate figures for excess deaths in weeks 14 to 18 of 2020 compared with the average for the previous five years in Britain and Europe have shown a spike well above the normal excess deaths for those weeks. The likelihood is that most of those excess deaths were caused either by the SARS-COV2 virus itself or by consequences of the lockdowns, such as a sharp reduction in normal surgical interventions.
Compare directly the flu positives for weeks 14-18 of 2020 with the corresponding weeks from 2019. For the same 11 countries, over those five weeks the number of flu positives was just 1,550 in 2020, but it was 12,934 – more than eight times greater – in 2019. That 88% reduction in flu positives is an indication that the lockdowns may be inhibiting the usual transmission of flu:
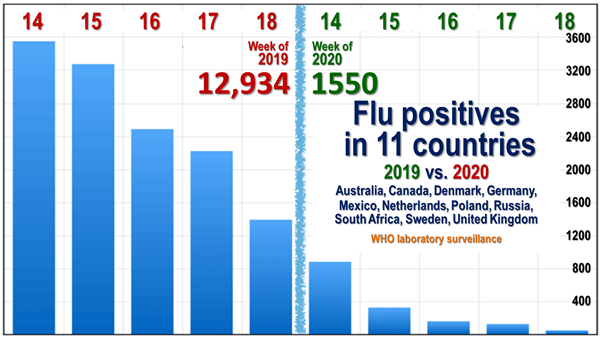
Looking just at week 14, six more countries can be added. Then the 2020 reduction is 90.9%:

The difference between reported flu positives in 2019 and 2020 becomes still more stark if the analysis is confined to the 14 countries meeting our criteria that have updated their data to week 17 of 2020 (Fig. 4):
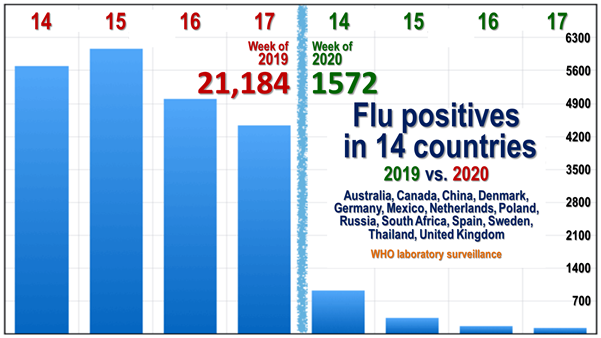
Here, the reduction in positive laboratory influenza test notifications over the two comparable periods is an impressive 92.6%.
Naturally, there are many confounders. Ideally one would want to average the previous five years’ data for weeks 14-18. And one would want to discover whether under-reporting of flu cases has increased because health personnel are busy coping with the pandemic. Nevertheless, the figures suggest that lockdowns do achieve their primary purpose, which is to reduce the transmission of infections.
As more data become available, it will be possible to make direct comparisons between both cases and deaths from flu and from the new infection. From the point of view of ending lockdowns, the comparison should be age-based because it is possible that for those under 60, and certainly for those under 50, the new infection is less fatal than flu.
It’s worth a closer look at influenza test positive results from several countries:
| Australia | China | Japan | Russia | Spain | UK | USA | |
| Week(s) | 14-18 | 14-17 | 14-16 | 14-18 | 14-18 | 14-18 | 14 |
| 2020 | 29 | 63 | 2 | 924 | 67 | 49 | 215 |
| 2019 | 852 | 9250 | 449 | 926 | 1541 | 2262 | 6903 |
| % fall | 96.6% | 99.3% | 99.6% | 0.2% | 95.4% | 97.8% | 96.9% |
The Russian results are an interesting outlier because Putin didn’t get serious about a lockdown until late March. That is a good indication that lockdowns work well and are the easiest to bring to an end if they are imposed early.
Russia’s flu positives were 537 in week 14, 231 in week 15, 99 in week 16, 47 in week 17 and 10 in week 18, from which I deduce Russia should soon start reporting a reduction in COVID-19 cases.
However, the UK and USA have been criticised for a perceived slow lockdown reaction to COVID-19, and Sweden had a 95.7% reduction in positive influenza test results comparing weeks 14-18 in 2019 and 2020 (1,541 > 67) despite only a partial lockdown.
Ignoring numerous other confounders such as population age and density, these discrepancies suggest some questions might be asked about the efficacy of lockdowns. However, laboratory flu test results from most countries indicate that social isolation has suppressed the spread of communicable diseases other than COVID-19, and this logically is evidence that lockdowns have done the same with the coronavirus itself.
These results cover just over a third of the world’s population from 17 different countries.
Therefore, if positive laboratory influenza tests are a moderately accurate reflection of infection percentages in their broader communities, and if influenza is a common indicator of community infection among the several dozen other communicable diseases, it might be said that the COVID-19 lockdowns have resulted in a ~90% reduction in global infections.
It may prove to be a lower percentage reduction, possibly dependent upon learned social distancing practices after lockdowns are lifted and the spread speed of different diseases, but the WHO influenza evidence suggests lockdowns have public health benefits beyond the targeted COVID-19.
- I am grateful to Lord Monckton for assistance in preparing the graphs.
So in my home I have several children. We are pretty certain that two of them have had the flu over this time period. However we have not gone in to have it diagnosed. Why? Because it would mean potential exposure to an environment where there is supposedly a highly infectious disease. Why would you, unless the person is REALLY REALLY sick go in?
I know there was mention of confounding factors but this is one of them. In my opinion you SHOULD see a lowering of the flu tests. Not only that but in my state you can go in and be tested for Covid if you have 1 ) a fever, and 2 ) an additional symptom. They then test you to see if you have Covid 19. Right now the test rate is coming back at 95.8% Negative for Covid 19. BUT they are not attempting to figure out WHAT the correct diagnosis should be ( Flu? )
While I appreciate the attempt to see if the lowering of communicable illness has dropped I think this is more of a case of Covid-19 taking the wind out of the sails of other testing. They are not testing for BOTH only for ONE, at least where I am. It would be interesting to see how many of the NEGATIVE covid tests would later show up as positive flu…
Chris Gillham
In attempting to suppress an epidemic, ideally, the government would use the most effective approach. Unfortunately, there are many reasons, such as cost, or an uncooperative population, why some compromise is going to be necessary.
This analysis doesn’t address the most important question of whether strictly enforced (e.g. welding doors shut) lockdowns are significantly more effective than willful social distancing. Indeed, even a binary distinction between lockdowns and social distancing is not defined. Preferably, a spectrum of responses would be provided so that the dependent variable (e.g. new cases) could be compared to the independent variable, number of potential contacts.
As long as nebulous terms are discussed, it will be impossible to sort out the confounding factors and reach any sort of reliable conclusion. About all that can be derived from your presentation is that when a country tries to do something to reduce transmission, some apparent effect can be measured; whereas, doing nothing, officially, results in widely disparate case and death rates between different countries.
It is obvious that the fewer person-to-person contacts there are, the fewer transmissions and new infections will take place. However, confining people to small quarters may not be the best way to accomplish that. For example, assume that one person in a household of 4 goes out to shop for groceries and somehow is infected. They then bring back the infection in person or on the purchased items. Then, everyone is exposed to the fresh virus. What has happened in prisons and elder care facilities makes the point that people confined in small areas are most at risk. It is generally accepted that the probability of infection is a function of the number of viruses, which in turn is a function of the concentration of viruses and the amount of time one is exposed to the source. Viruses on hard surfaces die within a matter of hours to, at most, days, even if not purposely disinfected. Having other members of a household gone for several hours while at work, could provide some protection.
However, the most important consideration is that strict lockdowns cannot be maintained indefinitely. It might be necessary for society to accept some upfront loss of life to avoid a collapse of the economy and the infrastructure supplying food. The lockdowns/social-distancing were initially rationalized on a need to prevent an overload of hospital resources. That has apparently been accomplished in all but maybe Italy. Further damage to economies is not warranted by your analysis.
Two important points that need addressed: First, the reporting delays that are typically associated with the collection of this information and secondly, the number of influenza tests actually performed this year as opposed to previous years. If only COVID-19 tests are being given at this point for symptomatic patients, then the flu numbers mean very little. Of course, the assumption would only be a logical one.
By Chris Gillham
“As one of the audit team for Jo Nova’s blog”
Pardon my ignorance, but what does a “audit team for Jo Nova” do?
In the absence of an answer I will assume Jo Nova’s audit team decides which comments are “relevant” to a particular post and consequently survive moderation, and which comments are not published.
PMHinSC,
Absolutely wrong.
No censorship exists within this group.
Never has,
There is some concordance of ideas, namely sound ones are preferred to stupid ones.
Geoff S (Member)
Geoff S,
Thank you for the reply. It was not my intent to offend; I am truly curious. I confess that I still do not know what the “audit team” does.
Regards.
Again, having received no reply, I will assume that what the Jo Nova Audit Team does is a secret and I will move on. Best to all.
This is just silly. Anyone with Influenza Like Illness (ILI) after March 2020 would never get tested for flu. They would get tested for Covid-19, told the test was negative and sent home. So you should add the Covid-19 negative count to the totals for March onwards.
It is an interesting theory, but to do this properly you’d need to look at hospital testing data and not Lab data. So compare total hospitalizations for ILI and subtract Covid-19 positive and compare to prior years total ILI activity.
Graphing the Missing Influenza Cases for late March and April 2020:
https://hailtoyou.wordpress.com/2020/04/29/against-the-corona-panic-pt-vi-where-has-the-regular-flu-gone-the-cdc-reports-unprecedented-crash-in-non-covid-flu-positives-raising-questions/
We are told that the Wuhan Coronavirus is spreading steadily. But “what happened to all the other seasonal virii that afflict humans this time of the year? Where did they all go?”
Hail
You asked, “Where did they all go?”
As is often the case, the US seasonal flu peaked in February, before COVID-19 really ramped up.
Chris Gillham
> “I have selected 17 countries based partly on their population size and prominence over the past few weeks in the COVID-19 crisis, and partly on whether or not they supplied sufficient weekly reports within the timeframe”
So, not Taiwan then. Nova avoids this example too – suits her propaganda, I think.
Taiwan has a death rate for C-19 per 10 million population of less than 1/13th of Australia’s. Almost the same population level (23m as against 25m), a much more intense population density as the Taiwanese island is so geographically tiny, and – drum roll – NO lockdown.
No wonder you avoid choosing it as an example. Yes, I know you are excluding C-19, but Taiwan also dealt with SARS-1, while Australia did not.
here
https://www.endcoronavirus.org/countries
“SOME ARE WINNING – SOME ARE NOT – a bunch of C-word social engineers”
Mind numbingly stupid, insultingly dumbed down gas-lighting!
Where is the larger but missing mountain of exposure, the endemic spread before the pandemic* that must have peaked at least 14 days prior to all those idiotic graphs – that list only the symptomatic – the so-called “cases”?
*The missing curve that represents the presymptomatic, the asymptomatic and those with non-specific and mild symptoms as well as any carriers or superspreaders!
Can we trust Covid modelling? More evidence from Sweden
https://www.spectator.co.uk/article/can-we-trust-covid-modelling-more-evidence-from-sweden
Dear Chris,
Why would you start you analysis at week 14 of 2019? If you would have started in week 1 of 2019, you would have had more overlapping weeks plus you would also cover the flu-peak in the first two months of the year.
Just wondering….
Since Jo Nova is an ardent proponent of ‘hard’ lockdowns, I suspect this article is not entirely objective.
You can’t compare influenza and Covid19 as done in this blog post because influenza isn’t very contagious. To understand this statement, read these two articles.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2870528/
https://virologyj.biomedcentral.com/articles/10.1186/1743-422X-5-29
> And one would want to discover whether under-reporting of flu cases has increased because health personnel are busy coping with the pandemic.
Or, a higher % of people who have flu-like symptoms are being tested for the flu becsuee they think they might have COVID-19.